Principles of Conventional & Alternative Therapy in Mastitis: A Comprehensive Review
Published: April 29, 2015
By: Dr. Zafar Ahmad & Dr. Garima Sinha (Natural Remedies Pvt. Ltd, Bangalore)
Major advances in the fields of animal breeding, animal nutrition and husbandry practices have played a significant role in increasing the global milk yield over the last two decades meeting the overwhelming demand for milk and milk products. There have been continuous changes in the predominance of etiological of mastitis greater understanding of the host responses to intra-mammary infections and treatment regimens leading to adoption of various control and prevention measures. Regardless, the problem of mastitis continues to pose the greatest challenge to the dairy industry worldwide.
Mastitis is the most dreaded disease of dairy animals which has huge impact on economics of a dairy farm. The related losses are associated with reduction in yield, increased treatment costs, discarded milk, and increase in culling and associated dairy cow replacement rates.
Therapeutic intervention is an important part of a control program for bovine mastitis. Therapy of infectious disease should either assist host defenses in eliminating invading pathogens or reduce the pathophysiologic consequences of infection.
1. Antibiotic Therapy
For antimicrobial therapy with either a parenteral or intramammary preparation, or the concurrent use of both types of preparation, to be effective an antimicrobial concentration exceeding the MIC for the causative pathogenic micro-organism must be maintained at the site of infection for an adequate duration.
a. Parenteral administration
Severe mastitis is usually treated systemically, although intramammary therapy will often be used adjunctively. The goal of antibacterial therapy is to attain effective concentrations of the drug at the site of infection.
For bovine mastitis, there are three potential therapeutic targets, or pharmacologic compartments.
The first (and most commonly targeted compartment) consists of the milk and the epithelial lining of the ducts and alveoli of the mammary gland. Pathogens (Streptococcus agalactiae, Streptococcus dysgalactia, coagulase-negative staphylococci) that typically reside in this compartment are generally noninvasive and are not believed to cause abscess formation in the parenchyma.
Second compartment consist the deep tissue of the mammary gland. Systemic administration is typically indicated for pathogens such as Staphylococcus aureus or Streptococcus uberis that are invasive or create abscesses
Third compartment of mastitis therapy: the cow as bacteremia can occur as a consequence of coliform mastitis
b. Intramammary administration
Intramammary route is accepted as the route of choice in the treatment of subclinical, chronic or mild clinical mastitis and as prevention during dry cow therapy.
Limitations of Intramammary administration
For the treatment of clinical mastitis only intramammary administration of antimicrobials is not sufficient to cure the animal completely because this route has some limitations like;
- Most of intramammary administration are used against gram-positive cocci and thus, have little or no activity against gram-negative pathogens.
- Intramammary infusion if not prepared under sterile conditions can result in supra-infections caused by secondary invaders.
- Limitations of intramammary administration with chronic IMI. Fibrin casts and micro abscess formation interfere with distribution of infused drugs to the site of infection in the terminal alveoli.
- Furthermore, the typical 24-hour to 36-hour duration of therapy for intramammary infusions limits the time period of effective concentration in the gland necessary to eliminate more chronic or invasive IMI.
2. Supportive therapy in bovine Mastitis- Beyond antibiotics what else we can do?
A multitude of mastitis therapies have been used before and after the advent of antibiotic therapy. Most alternative therapies are aimed at helping the cow’s own defence mechanisms to clear the infection rather than attacking the pathogen directly as is the case with antibiotics.
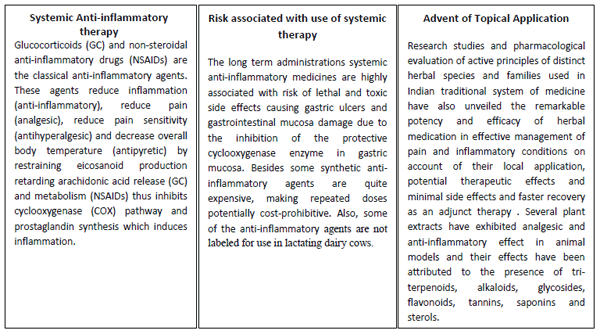
a) Anti-inflammatory Therapy
An important aspect of mastitis therapy is the alleviation of inflammation in the udder. Swelling and subsequent pain associated with clinical mastitis can cause considerable discomfort to the cow. Antibiotic preparations offer no immediate relief from pain.

b. Oxytocin: Milk is the rich medium for the growth of microorganisms; hence it should be removed from the affected quarters at every 3-4 hours. Oxytocin used to facilitate complete milk evacuation and to remove toxic material and debris.
c. Fluid therapy: Isotonic fluids containing glucose and antihistaminic are to be used in per acute and acute cases with extensive tissue damage and toxaemia.
d. Nutritional supplements
The quality and plan of nutrition appears to be an important factor that influences clinical manifestation of mastitis in heifers and cows
Vitamin E is one of the important supplements in dairy feed to boost the immune response of cows and to enhance the neutrophil function. Vitamin E is often combined with selenium, which acts as an anti-oxidant by preventing oxidative stress.
Beta-carotene and Vitamin A are effective in preventing the occurrence of mastitis due to their antioxidant and immune-enhancing properties and contribution in mucosal surface integrity of the mammary gland respectively.
Zinc and copper are also important nutritional elements that contribute mammary gland health by promoting cellular repair, wound healing and reduction in SCC aided by increasing metallothionein synthesis with antioxidant potential.
Suggested levels of supplementation (amount/cow/day)
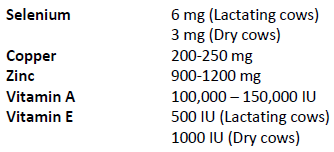
e. Immunomodulators
Some of the herbal immunomodulator like tulsi (Ocimum sanctum) have better effect to enhance immune system to fight against mammy gland infection. Levamisole is one of the well-known immunomodulator which can enhance the immune power of animal to fight against diseases.
Conclusion
Treatment is an important aspect of mastitis control. The most effective treatment strategies include early detection, presumed identification of mastitis pathogens and the use of antibiotics for an appropriate duration for the expected pathogen. Despite the widespread use of various antibiotics and other chemotherapeutic agents, antibacterial treatment of mastitis has generally achieved less than the desirable result. The pathology of the udder tissue caused by mastitis and its effect on the pharmacokinetic properties of mastitis drugs, widespread antibiotic resistance, appears to be a major cause of therapy failure. Success of mastitis therapy is lower in lactating dairy cows than in dry cows. Poor animal husbandry and veterinary practice also contribute to a less favourable prognosis. The answer to the mastitis problem lies in eliminating or minimizing the predisposing factors to mastitis and in the prevention of new intramammary and teat canal infections in association with accurate treatment regimen followed for the existing mastitis cases and infections.
Related topics:
Authors:
Natural Remedies Private Limited
Recommend
Comment
Share
11 de mayo de 2015
Helllo Dr Zafar and others, I would like to suggest you to please go through our article published in 'Engormix' sometime ago entitled 'Pathobiology, etiology and treatment of mastitis in buffaloes" by KS Dhillon, Jasmer Singh from Punjab Agricultural University, College of Vety. Sciences, Ludhiana. This article provides details of the cause of mastitis and its radical cure/control in dairy animals. There are some pharmaceuticals which have come out with preparations for the control of mastitis. The basic cause of mastitis in dairy animals is the problem of citrate synthesis in the udder. The main functions of citrate in udder are: 1. Maintain normal pH (~6.50) of udder, 2. Sequester Calcium (Ca++) in milk and preserve the fluidity of milk. In citrate deficiency everything proceeding in concert goes haywire and the result is mastitis. This ailment can be effectively controlled by the administration of Trisodium citrate -30gms dissolved in about 100ml of water as a drench once daily till cure-which takes usually 3-4 days. The sterile solution of this salt can also be used I/V as 10 % given 50ml at a time followed by oral administration as mentined above. This treatment restores the normal pH and prevents flake formation which are the "Hallmarks" of mastitis. For any further discussion on any aspect of this economically most important disease any body is most welcome.
Jasmer Singh Ph D
Recommend
Reply
Recommend
Reply
30 de octubre de 2015
Thanks a lot Dr. Dr. Zafar Ahmad & Dr. Garima Sinha for this valuable information.
Recommend
Reply
12 de agosto de 2015
Dear colleagues; it is really nice information and discussion on mastitis treatment and prevention that explained well. I would like to translate some parts for those of my colleagues who have language difficulties in English, on local language in My country / Afghanistan .
thanks
Dr. Abdul Qader Samsor
Recommend
Reply


BOVIMIN – GL
BOVIMIN–GL are Glycine chelated minerals to improve conception rate, Reduces cow open day, Improves pregnancy rate, prevent Masitis, all in dairy cattle
Suggested link
Recommend
Reply
Recommend
Reply
5 de mayo de 2015
Thanks Dr.Zafar for the beneficial artice
As you concluded preventive measures is the key factor to reduce percentage of subclinic mastitis in dairy herds from vaccination to good hygiene and proper feeding. Subclinic mastitis is like iceberg we can not see accurately it's submerged part. Treated cows must be observed for a long time as an infection source.
Recommend
Reply

Would you like to discuss another topic? Create a new post to engage with experts in the community.
Featured users in Dairy Cattle

José Manuel Oropeza Meza
MSD - Merck Animal Health
Gerente Nacional Cuentas Clave en MSD Salud Animal
United States
United States













