Mycoplasma bovis pneumonia in feedlot cattle and dairy calves in Argentina
1 Grupo de Sanidad Animal, Estación Experimental Agropecuaria INTA Marcos Juárez, Córdoba, Argentina; 2 Facultad de Ciencias Veterinarias, Universidad Nacional de Rosario, Casilda, Santa Fe, Argentina; 3 Servicio Central de Microscopía Electrónica, Facultad de Ciencias Veterinarias, Universidad Nacional de La Plata, La Plata, Buenos Aires, Argentina; 4 Instituto de Virología, CICVyA, INTA Castelar, Morón, Buenos Aires, Argentina; 5 College of Veterinary Medicine, Western University of Health Sciences, Pomona, California, USA; 6 Department of Pathology and Microbiology, Atlantic Veterinary College, University of Prince Edward Island, Charlottetown, Prince Edward Island, Canada.
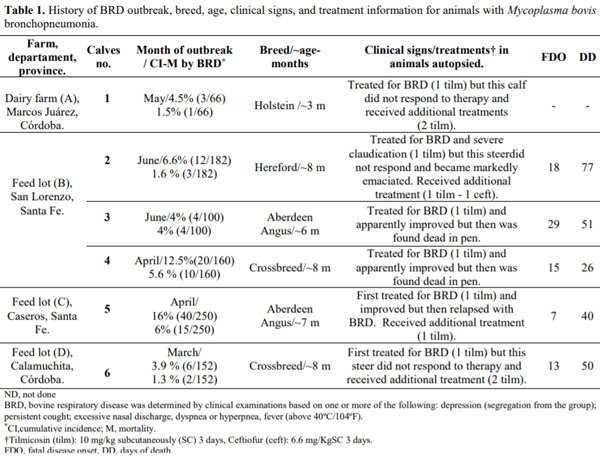
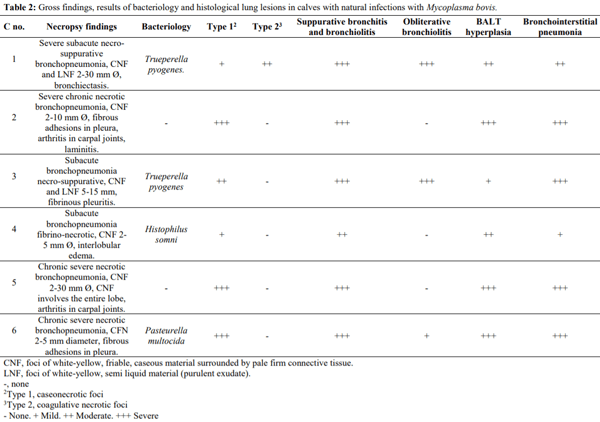
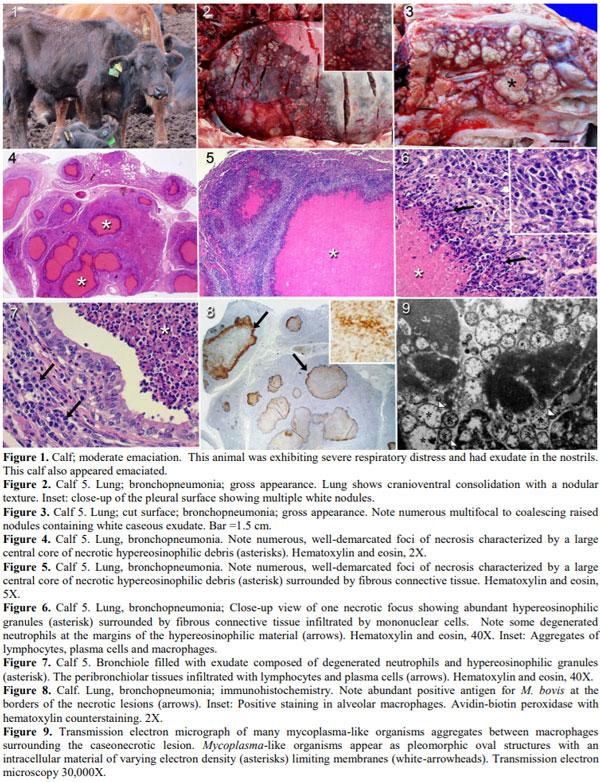
Mycoplasma bovis has emerged as an important cause of feedlot pneumonia in many countries. The aim of this paper is to describe six cases of bovine Mycoplasma pneumonia in five different premises in Argentina. Gross examination revealed chronic bronchopneumonia with multiple foci of caseous necrosis. Microscopically, these contained a necrotic center with abundant hypereosinophilic granular material surrounded by granulation tissue. Affected lung tested positive for M. bovis by immunohistochemistry and electron microscopy revealed membranous structures compatible with Mycoplasma spp. To our knowledge, this is the first report of M. bovis pneumonia in Argentina.
Key words: chronic bronchopneumonia, electron microscopy, feedlot, immunohistochemistry, Mycoplasma bovis.
- Adegboye DS, Halbur PG, Nutsch RG, Kadlec RC, Rosembusch RF. Mycoplasma bovis-associated pneumonia and arthritis complicated with pyogranulomatous tenosynovitis in calves. J Am Vet Med Assoc. 1996;209:647-9.
- Arcangioli MA, Duet A, Meyer G, Dernburg A, Be´zille P, Poumarat F, LE GRAND D. The role of Mycoplasma bovis in bovine respiratory disease outbreaks in veal calf feedlots. Vet J. 2008;177:89-93.
- Ayling RD, Baker, SE, Peek ML, Simon AJ., Nicholas RAJ. Comparison of in vitro activity of danofloxacin, florfenicol, oxytetracycline, spectinomycin and tilmicosin against recent field isolates of Mycoplasmabovis. Vet Rec. 2000;146:745-7.
- Bell C.J, Blackburn P, Elliot M, Patterson TIAP, Ellison S, Lahuerta-marin A, Ball HJ. Investigation of polymerase chain reaction assays to improve detection of bacterial involvement in bovine respiratory disease. J Vet Diag Invest. 2014;26:631-4.
- Booker CW, Abutarbush SM, Morley PS, Jim G.K, Pittman TJ, Schunicht OC, Perrett T, Wildman BK, Fenton RK, Guichon PT, Janzen ED. Microbiological and histopathological findings in cases of fatal bovine respiratory disease of feedlot cattle in Western Canada. Can Vet J. 2008;49:473-81.
- Bürki S, Frey J, Pilo P. Virulence, persistence and dissemination of Mycoplasma bovis. Vet Microbiol. 2015;179:15-22.
- Carter GR. Diagnostic procedures in veterinary bacteriology and mycology. 4th ed. Springfield: C.C. Thomas; 1984. 515 p.
- Caswell JL, Williams KJ. Respiratory system. In: Maxie MG, editor. Jubb, Kennedy and Palmer’s Pathology of Domestic Animals. 6th ed., vol. 2. St. Louis: Elsevier; 2016. p. 465-591.
- Caswell JL, Archambault M. Mycoplasma bovis pneumonia in cattle. Anim Hlth Res Rev. 2008;8:161-86.
- Caswell JL, Bateman KG, Hugh YC, Castillo-Alcala F. Mycoplasma bovis in respiratory disease of feedlot cattle. Vet Clin North Am Food Animal Pract. 2012;26:365-79.
- Cerdá R, Xavier J, Sansalone P, De La Sota R, Rosembusch R. Aislamiento de Mycoplasma bovis a partir de un brote de mastitis bovina en una vaquería de la provincia de Buenos Aires. Primera comunicación en la República Argentina. Rev La Am Microbiol. 2001;42:7-11.
- Ellis JA. The immunology of the bovine respiratory disease complex. Vet Clin North America Food Anim Pract. 2001;17:535-50.
- Francoz D, Fortin M, Fecteau G, Messier SE. Determination of Mycoplasma bovis susceptibilities against six antimicrobial agents using the E test method. Vet Microbiol. 2005;105:57-64.
- Fulton, RW, Blood SK, Panciera RJ, Payton ME, Ridpath JF, Confer AW, Saliki JT, Burge TL, Welsh RD, Johnson BJ, Reck A. Lung pathology and infectious agents in fatal feedlot pneumonias and relationship with mortality, disease onset, and treatments. J Vet Diagn Invest. 2009;21:464-77.
- Gagea MI, Bateman KG, Van Dreumel T, Macewen BJ, Carman S, Archambault M, Shanahan RA, Caswell JL. Diseases and pathogens associated with mortality in Ontario beef feedlots. J Vet Diagn Invest. 2006;18:18-28.
- Haines DM, Chelack BJ. Technical considerations for developing enzyme immunohistochemical staining procedures on formalin-fixed, paraffin-embedded tissues for diagnostic pathology. J Vet Diagn Invest. 1991;3:101-12.
- Haines DM, Martin KM, Clark EG, Jim J, Janzen ED. The immunohistochemical detection of Mycoplasmabovis and bovine viral diarrhea virus in tissues of feedlot cattle with chronic, unresponsive respiratory disease and/or arthritis. Can Vet J. 2001;42:857-60.
- Hermeyer K, Buchenau I, Thomasmeyer A, Baum B, Spergser J, Rosengarten R, Hewicker-Trautwein M. Chronic pneumonia in calves after experimental infection with Mycoplasma bovis strain 1067: characterization of lung pathology, persistence of variable surface protein antigens and local immune response. Acta Vet Scand. 2012;54:1-11.
- Horwood PF, Schibrowski ML, Fowler EV, Gibson JS, Barnes TS, Mahony TJ. Is Mycoplasma bovis a missing component of the bovine respiratory disease complex in Australia? Aust Vet J. 2014;92:185-91.
- Khodakaram-Tafti A, López A. Immunohistopathological findings in the lungs of calves naturally infected with Mycoplasma bovis. J Vet Med A Physiol Pathol Clin Med. 2004;51:10-4.
- Kleinschmidt S, Spergser J, Rosengarten R, Hewicker-Trautwein M. Long-term survival of Mycoplasmabovis in necrotic lesions and in phagocytic cells as demonstrated by transmission and immunogold electron microscopy in lung tissue from experimentally infected calves. Vet Microbiol. 2013;162:949-53.
- López A, Martinson SA. Respiratory System, Mediastinum, and Pleurae. In: Zachary JF, editor. Pathologic Basis of Veterinary Diseases. 6th ed. St. Louis: Elsevier; 2017. p. 471-560.
- Nicholas RAJ, Ayling RD. Mycoplasma bovis: disease, diagnosis, and control. Res Vet Sci. 2003;74:105-12.
- Panciera R, Confer AW. Pathogenesis and pathology of bovine pneumonia. Vet Clin North America Food Anim Pract. 2010;26:191-214.
- Radaelli E, Luini M, Loria GR, Nicholas RAJ, Scanziani E. Bacteriological, serological, pathological and immunohistochemical studies of Mycoplasma bovis respiratory infection in veal calves and adult cattle at slaughter. Res Vet Sci. 2008;85:282-90.
- Ramírez-Romero R, Chavarría-Martínez B, Nevárez-Garza, AM, Rodriguez-Tovar LE, Dávila-Martinez C, Hernandez-Vidal G, Hernandez-Escañero JJ, Lopéz-Mayagoitia A. Demostración histoquímica de Mycoplasma bovis en lesiones neumónicas crónicas en ganado de corral de engorda.Vet Mex. 2010;41:289-96.
- Rodriguez F, Bryson DG, Ball HJ, Forster F. Pathological and immunohistochemical studies of natural and experimental Mycoplasma bovis pneumonia in calves. J Comp Pathol. 1996;115:151-62.
- Rodriguez F, Kennedy S, Bryson TD, Fernandez A, Rodirguez JL, Ball HJ. Immunohistochemical method of detecting Mycoplasma species antigen by use of monoclonal antibodies on paraffin sections of bovine and caprine lungs. Zentralbl Veterinarmed B. 1996;43:429-38.
- Rosenbusch, RF, Kinyon JM, Apley M, Funk ND, Smith S, Hoffman JL. In vitro antimicrobial inhibition profiles of Mycoplasma bovis isolates recovered from various regions of the United States from 2002 to 2003. J Vet Diagn Invest. 2005;17:436-41.
- Terlaak EA, Wentink GH, Zimmer GM. Increased prevalence of Mycoplasma bovis in the Netherlands. Vet Quart. 1992;14:100-4.
- Thomas A, Nicolas C, Dizier I, Mainil J, Linden, A. Antibiotic susceptibilities of recent isolates of Mycoplasma bovis in Belgium. Vet Rec. 2003;153:428-31.
- Yilmaz R, Cangul IT, Onat K, Akkoc A, Ozyigit MO, Akdesir E. Histopathological, immunohistochemical and bacteriological characterization of Mycoplasma bovis pneumonia in cattle. Pakistan Vet J. 2016;36:316-21.











